Leg Ulcers
The below content has been medically reviewed and approved by Consultant Interventional Radiologist Dr. Mark Bratby (MBBS, MRCP, FRCR), Medical Director and Head of the Medical Advisory Committee at VeinCentre.
Last reviewed 1st August 2024.
Overview of Leg Ulcers
Here at VeinCentre, we have almost 20 years’ experience in treating venous leg ulcers via EVLA and foam sclerotherapy. We find that these methods lead to quicker healing and longer-lasting results (they tend to remain healed) in comparison to traditional methods like only applying compression bandaging.
A leg ulcer is any break in the skin, usually found on the lower part of the leg or the feet. They are typically diagnosed on their appearance, which in itself can be confusing as they can have so many different appearances. Leg ulcers develop when an area of skin breaks down to reveal the tissue underneath. Venous ulcers are the most common type of leg ulcer, accounting for over 60% of leg ulcers according to NHS statistics. It is estimated that the condition affects as many as 1 in 500 people in the UK with 1 in 50 adults over the age of 80 having an ulcer. They mainly occur just above the ankle and are often very painful.
The NHS treatment for venous ulcers remains a cleaning and dressing procedure, complete with compression, performed in the community, over a long period of time. There is inconsistency in referring patients with leg ulcers for assessment of their veins and the referral pathways in the NHS take a considerable time before patients arrive at the doorstep of a vascular specialist. Without addressing the underlying cause of the condition timely, healing can be delayed, and recurrence rate is high.
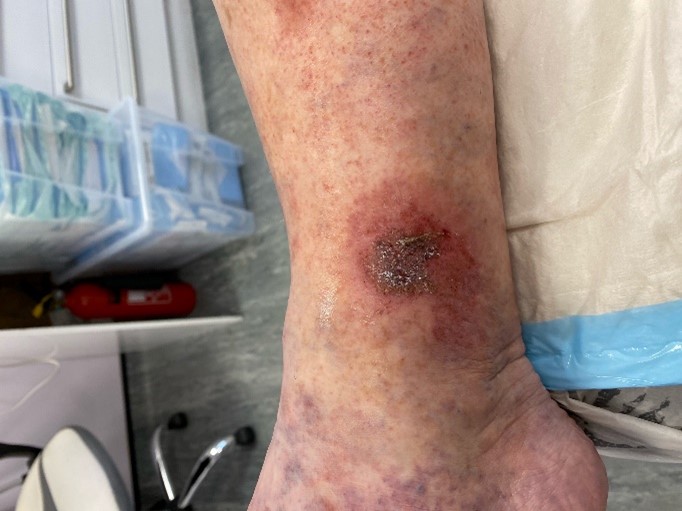
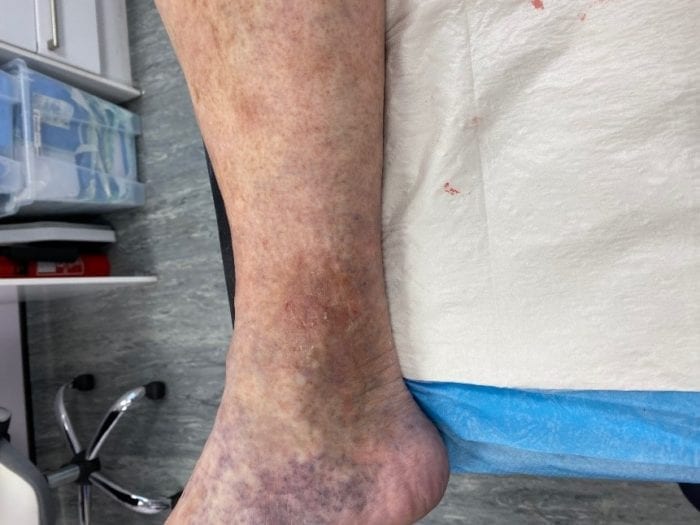
Leg Ulcers Symptoms
Venous leg ulcers are open sores, usually found on the lower leg, that can be painful and slow to heal.
Typical symptoms which may manifest themselves include varicose veins, varicose eczema, swollen ankles, a feeling of heaviness in the legs, discolouration or hardening of the skin and achy legs. Some leg ulcers may also have a nasty-smelling discharge.
Some of those symptoms are worsened when the patient is sitting or standing, as the leg is below the heart, amplifying the effect of the venous insufficiency. In contrast, those patients who are able to rest either lying down or with their leg elevated show signs of those symptoms easing as gravity works with the body to move blood back to the heart.

We are processing your answers – hold tight!
Complete Quick Online Assessment
Leg Ulcers Causes
Fundamentally, leg ulcers are caused by increased blood pressure caused by problems with the circulation of blood in the leg veins. The skin of the leg can gradually get damaged and can be made fragile by the constant high pressure (venous hypertension).
This is usually due to valve failure, which is the normal cause of varicose veins. In our experience most patients with venous leg ulcers will also have varicose veins (or have a history of them).
Leg Ulcers Diagnosis
At VeinCentre, your consultation will begin with a conversation with your consultant. They will then undertake an ABPI test which will confirm whether or not the ulcer is venous, as we only treat venous ulcers at Veincentre. With the confirmation that the ulcer is venous, the consultant will perform a colour duplex ultrasound scan on your legs from your feet up to your groin. This scan is the only way to accurately identify whether there is a venous problem causing the ulcer (i.e. varicose veins).
Leg Ulcers Prevention
If you believe that you are at risk of developing venous ulcers, you can make changes to your lifestyle to potentially help prevent their onset. Getting regular exercise, eating healthily, and getting enough sleep to feel rested, perhaps to aid losing weight, may help improve blood flow in both arteries and veins. If you are a smoker, quitting will take some of the strain off your cardiovascular system, which in turn can help the circulation.
Leg ulcers do present early signs that may not be recognised by many. The skin of the lower leg can become discoloured and turn into a brown patch, usually on the inside of the area. If left untreated this can turn to a dark brown patch and eventually become ulcerated.
Traditionally, GPs have suggested that compression bandaging or compression stockings to help to improve circulation within the affected area, encouraging blood flow from the feet to the heart. Whilst compression therapy is vital part of managing venous ulcers, at Veincentre we believe that the best way to prevent the development and recurrence of venous leg ulcers is to treat the underlying cause with EVLA.
In most cases, after the ulcer has healed post-EVLA, it will not be necessary to wear compression stockings, which means that you can get on with your normal life.
Treatment
At VeinCentre, our treatment pathway for leg ulcers is similar to that for varicose veins. Leg ulcer treatment would start with an ABPI test and a duplex ultrasound scan, performed during your consultation, to confirm whether the ulcer is venous and to determine if there is an underlying cause your venous ulcers (i.e. varicose veins). From that scan and the knowledge that your ulcer is venous, the best course of treatment is defined for your case, tailored specifically to your condition.
We suggest that treating varicose veins with EVLA will produce the best long term results. To find out about our treatments in more detail, please read here.
Once the treatment is complete and the veins have closed, the leg ulcer will heal relatively quickly as the underlying cause which led to the ulcer has been fixed. The wound will close up, the redness will fade and any eczema will begin to clear up.