Varicose Vein Treatment Risks
We are upfront and honest regarding the treatment risks. We encourage you to weigh up the treatment benefits vs. risks prior to treatment.
What can happen with varicose vein treatment?
This is a common concern, and rightly so. Nobody should enter into any medical treatment without being aware of the potential downsides as well as the benefits.
Perhaps surprisingly most vein clinic websites fail to highlight potential risks giving the impression that all treatments are perfectly safe with nothing at all to worry about. We are different. We are open and honest in our approach to our business and feel it is essential to warn potential patients of the small but real risk of side effects.
Compared to traditional surgical stripping, the newer, minimally invasive forms of varicose veins treatment are incredibly effective and safe. However, on rare occasions, problems have been known to occur, and you need to be aware of these when deciding whether or not to have treatment. Having said that, it is also important to be aware of the risks of doing nothing, as these risk of inaction, in many patients, are higher than the risks of treatment. Complicated, isn’t it?
You will be informed at your consultation about these risks, and if any are more likely in your particular case, we will discuss this with you.
What are the complications of our minimally invasive vein treatments?
Skin Staining
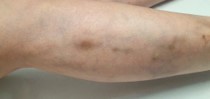
Skin staining can occur following either foam sclerotherapy or microsclerotherapy. This is not a risk to your health but can result in a disappointing cosmetic outcome particularly short-term, this will fade of a period of months and in 1-2% can take 12-18 months to fade. We can not guarantee there will never be any permanent marks but these are thankfully rare.
Occurs within 4-6 Weeks of treatment
60% resolve within 6 months
95% resolve within 1 year
1-2% have pigment > 1 year
VTE (Venous thromboembolism)
Deep vein thrombosis (DVT) and pulmonary embolus (PE) are uncommon after endovenous laser ablation (EVLA) and/or foam sclerotherapy. We continually audit DVT and PE and in 2023 the rates for both were less than 1 in a 1000. This is much lower than published studies, with typical rates of one in 200 for DVT, and one in 1,000 for PE.
DVT presents as a swollen (3cm > pre-treatment) painful calf and requires urgent review in urgent care (GP/out-of-hours) and usually you would be given a blood-thinner and a scan arranged the following day.
PE is a serious condition and needs to be urgently diagnosed and treated and can occur without leg swelling. Any new shortness of breath is a red-flag symptom and would warrant urgent review in A&E.
We will risk assess you for VTE and if there are risk factors you may be provided with either a single-dose of injected blood-thinner at the time of the procedure and some high-risk patients prescribed a week of additional blood-thinner medication, although this no complete guarantee we can prevent every blood clot and there are very small risks of significant bleeding with these medicines.
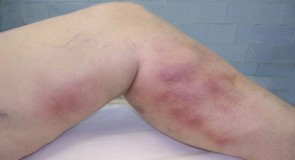
Phlebitis
Most patients will experience phlebitis (inflammation in a treated vein) after EVLA and/or sclerotherapy. This is usually self-limiting with mild discomfort.
Occasionally there can be quite severe pain and this can occur many weeks/months after initial treatment.
This is best managed with ibuprofen gel or tablets (but not both) and sometimes we can take some trapped blood out of the lumpy sore vein. The area can often be quite warm to touch but rarely requires antibiotics and will settle with anti-inflammatory medication.
Allergic reactions
Any exposure to a new drug could result in an allergic reaction, although serious allergic reaction is rare. Emergency drugs are stocked in all clinics to deal with a reaction.
Infection
As we are not making incisions in most cases, just needle punctures, the risk of infection is very low. We have seen one serious case that required antibiotics and hospital admission. If your procedure included avulsions, the size of your incisions may range from needle punctures to 3mm cuts and such incisions carry slightly higher risk of infection.
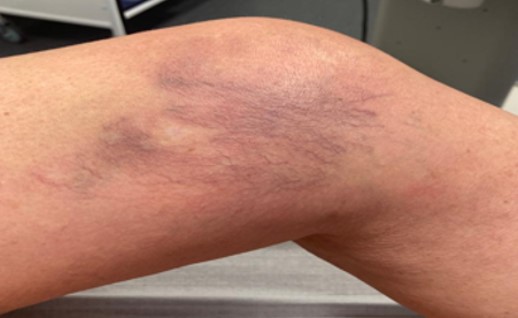
New thread veins
New thread veins can occur along the line of EVLA or after sclerotherapy or microsclerotherapy. We can mostly improve appearances with further microsclerotherapy. There is a rare condition called telangiectatic matting with profuse thread vein patches and redness usually on the inside of the knees. As with all thread veins some can be resistant to any further treatment.
Nerve damage
We have never seen any damage to a nerve that supplies muscles and therefore affects movement of the leg. This is exceedingly unlikely to happen. Nerves that transmit sensations from the skin can be damaged especially with EVLA below the knee and this can lead to numbness or tingling on the inside of the lower leg. This usually gets better in 3-4 months and is not disabling, although sometimes can be permanent leaving a numb patch of skin.
Visual disturbance/migraine
About one in 400 patients may develop a temporary visual disturbance similar to a migraine aura (flashing lights) immediately after treatment. This usually takes about 10 minutes to resolve, and we will monitor and support you in the clinic: all that is needed is reassurance and monitoring.
These are likely caused by tiny bubbles of sclerosant entering the blood supply to the brain. This sounds frightening, but we have never seen any long-lasting visual problems. The likelihood of these reactions increases in those with a history of migraine. Foam sclerotherapy can also trigger migraine attacks (although these can also be triggered due to stress from having a medical procedure).
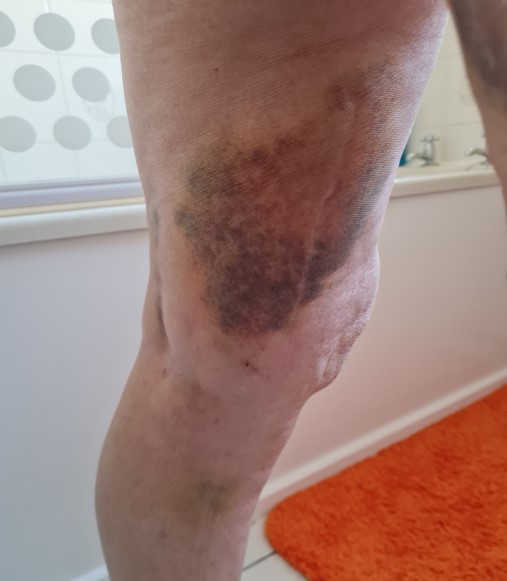
Bruising
Bruising will appear a few days after the treatment, and can in some cases appear quite extreme, particularly if you regularly take or are prescribed blood thinners. This will settle over a few weeks and is nothing to be alarmed by.
Stocking top reactions
Reactions to the stocking tops are quite common and is mostly due to the stocking being pulled too high and the elastic pulling on the skin every time the leg is bent. If there is skin irritation, the stocking top can be turned down or gauze placed between the skin.
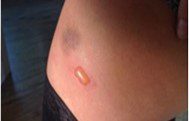
Skin ulceration
Skin marks such as blisters or even ulceration can occur, due to skin breakdown over a treated vein or irritation of skin from any of the treatments. This is particularly rare but require local dressings and could result in an area of scarring.
Bleeding/Haematoma
EVLA is performed through a “pinhole” skin access, and we sometimes see oozing onto the stocking. There can sometimes be significant bleeding or haematoma formation after avulsions.
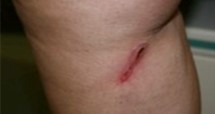
Skin burns
We have seen two cases of skin burns (see image below); however, these were both over 10 years ago in the early days of our practice and occurred after VNUS RF ablation. We have never seen any burns after EVLA laser treatment, but it is theoretically possible.
Skin burn after VNUS RF
Rare complications (<1/3,000)
Breakage of laser fibre or catheter.
We have had five cases where either the laser fibre or catheter were damaged during the procedure. These were all removed without any long-term problem.
Very Rare Complications (<1/10,000)
- Anaphylaxis (Severe life threatening allergic reaction)
- Heart attack
- Tissue necrosis (gangrene or death of skin/ muscle)
- Stroke
- TIA (minor stroke)
- Death
