Leg Ulcers
The below content has been medically reviewed and approved by Consultant Interventional Radiologist Dr. Mark Bratby (MBBS, MRCP, FRCR), Medical Director and Head of the Medical Advisory Committee at VeinCentre.
Last reviewed 16th December 2025.
At VeinCentre, we’ve been helping patients manage and heal venous leg ulcers for almost 20 years. Our experience shows that treating the root cause, often venous reflux, with clinically recommended procedures such as Endovenous Laser Ablation (EVLA) and foam sclerotherapy offers quicker healing and longer-lasting results. In many cases, once the underlying vein issue is treated, the ulcer begins to heal naturally and stays closed for good. Unlike traditional approaches that rely solely on compression bandaging, our minimally invasive treatments are designed to resolve the underlying cause rather than just manage the symptoms. If you’ve been living with a leg ulcer, we’re here to offer lasting relief with expert care and personalised support every step of the way.
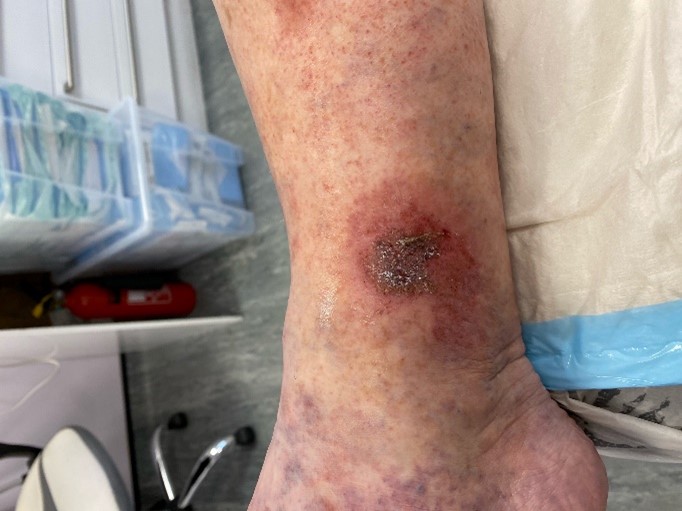
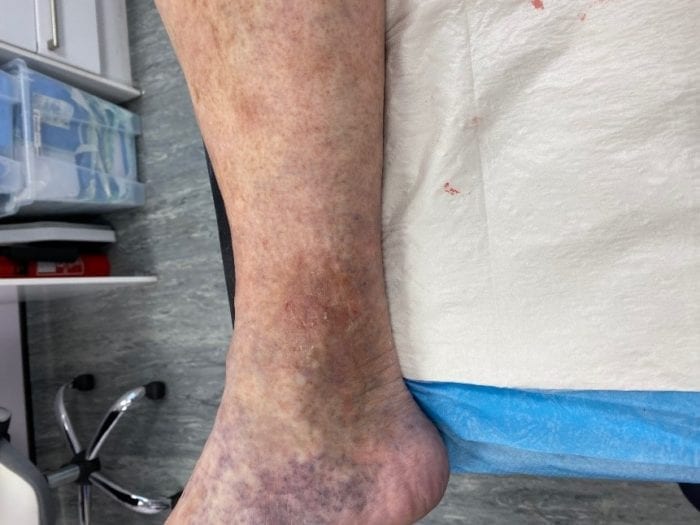
What are Leg Ulcers?
A leg ulcer is a break in the skin, usually found on the lower leg or foot, that takes time to heal. They can vary significantly in appearance, which can make the diagnosis feel a little confusing. Leg ulcers form when an area of skin becomes damaged and starts to break down, exposing the tissue underneath. Venous leg ulcers are the most common type, making up over 60% of all leg ulcer cases according to NHS data. It’s estimated that around 1 in 500 people in the UK are affected, with that number rising to 1 in 50 among adults over 80. They typically appear just above the ankle and can be very painful.
Many patients are still managed in the community with wound cleaning, dressings, and compression over long periods of time. While this can help with symptoms and healing, it does not always treat the underlying cause. Unfortunately, referrals for vein assessment on the NHS can take time, and many patients are not seen by a vascular specialist as early as they might need. Without treating the root cause, often venous reflux, healing can be slower, and ulcers are more likely to return.
At VeinCentre, we believe in taking a proactive approach by identifying and addressing the underlying vein issue with proven treatments like EVLA. This helps support faster healing and reduces the chance of recurrence, giving you the best chance of lasting relief.
Leg Ulcer Characteristics
Leg ulcers can vary in size, appearance, and severity, but they all have one thing in common: they’re wounds that struggle to heal on their own. Most venous leg ulcers develop just above the ankle and may start as a small area of irritated or damaged skin. Over time, this can break down to form a sore that remains open for weeks or even months.
You might notice symptoms such as aching or heaviness in the leg, swelling, hardened skin around the ulcer, or a feeling of tightness. The area may also look red, flaky, or shiny, and some ulcers can produce discharge or have an unpleasant smell if they become infected.
Because they develop slowly, leg ulcers can sometimes go unnoticed in the early stages. If you spot a wound that isn’t healing or is getting worse, it’s important to seek advice. A specialist scan can identify whether poor vein function is contributing to the problem, and if so, we can recommend effective treatment options to support healing and help prevent future issues.
Leg Ulcers Symptoms
Leg ulcers can come with a variety of symptoms, some of which may build gradually over time. Common signs include aching or heaviness in the legs, particularly after standing or sitting for long periods. You might notice swelling around the ankle, especially by the end of the day, or a persistent area of skin irritation that doesn’t seem to heal.
The skin around a developing ulcer may feel dry, itchy, or tight, and the area might appear red or discoloured. Some people experience a burning or throbbing sensation, while others may notice hardened skin or a rash. If the ulcer becomes infected, it could start to produce discharge or develop an unpleasant smell.
Because symptoms can vary, it’s important not to ignore changes in your skin or leg comfort. If you’re unsure or something doesn’t feel quite right, we’re here to help you get the answers and support you need.
Complete Quick Online Assessment
What Causes Leg Ulcers?
Leg ulcers are most commonly caused by problems with the circulation in your veins. When the tiny valves inside the veins stop working properly, blood can begin to flow the wrong way and pool in the lower legs. This increases the pressure in the veins – a condition known as venous hypertension, which can, over time, weaken and damage the surrounding skin.
As the skin becomes more fragile due to this ongoing pressure, even a minor knock or injury can result in a wound that struggles to heal. This is what leads to the development of a leg ulcer.
In many cases, this valve failure is the same underlying issue that causes varicose veins. In our experience, most patients who develop a venous leg ulcer will either have visible varicose veins or a history of them.
By understanding and addressing the root cause of venous issue, we can support proper healing and help reduce the chances of ulcers returning in the future. If you’re concerned about a persistent wound or changes to your skin, we’re here to help guide you through the next step.
How to Prevent Leg Ulcers?
If you’re concerned about your risk of developing a venous leg ulcer, the good news is that there are steps you can take to help protect your vein health. Making small but consistent changes to your daily routine can go a long way. Regular gentle exercise, such as walking, helps to keep your blood moving, while eating a balanced diet, staying well-hydrated, and getting enough rest all support your circulation. If you smoke, stopping can also have a big impact by reducing the strain on your cardiovascular system.
It’s also worth being aware of the early signs that can sometimes appear before a leg ulcer forms. You might notice a patch of brown or discoloured skin on the lower part of your leg, often on the inner side above the ankle. This is sometimes a sign of changes in the underlying veins and, if left untreated, can gradually worsen and break down into an ulcer.
GPs commonly advise compression therapy to support circulation and ease symptoms. Bandages or stockings help encourage blood to flow from your feet back up toward your heart. While this can help manage the condition, it does not treat the root cause.
At VeinCentre, we believe the most effective way to prevent leg ulcers and stop them from coming back is to treat the underlying vein problem. That’s why we use EVLA (Endovenous Laser Ablation), a minimally invasive procedure that targets the cause of venous ulcers. In our experience, once the vein issue is treated and the ulcer has healed, many patients no longer need to rely on compression stockings and can return to everyday life with confidence.
If you’ve noticed changes in your legs or are worried about developing an ulcer, we’re here to help you take the next step with clarity, comfort, and expert care.
Diagnosis & Consultation
Your journey with us begins with a relaxed, one-to-one conversation with your Vascular Consultant. We take the time to understand your symptoms, listen to your concerns, and explore how your leg ulcer is affecting your day-to-day life. This personal approach helps us tailor the next steps to your individual needs.
To begin the diagnostic process, your Consultant may carry out an ABPI (Ankle Brachial Pressure Index) test. This simple, non-invasive assessment measures the blood pressure in your ankles and arms to determine if your ulcer is caused by a venous issue. At VeinCentre, we specialise in treating venous leg ulcers, so this step is essential in confirming whether our treatments are right for you.
If the results show that the ulcer is venous, your consultant will then perform a detailed colour duplex ultrasound scan. This scan looks at the veins in your legs from your feet to your groin and is the only accurate way to detect underlying problems such as reflux or valve failure, the common causes of venous leg ulcers.
The entire consultation, including the ABPI and scan, is carried out during a single visit. By the end of your appointment, you’ll have a clear understanding of the cause of your ulcer, and we’ll talk you through your personalised treatment options, so you can feel confident and informed about your next steps.
Treatment Options
At VeinCentre, our treatment pathway for leg ulcers is similar to that for varicose veins. Leg ulcer treatment would start with an ABPI test and a duplex ultrasound scan, performed during your consultation, to confirm whether the ulcer is venous and to determine if there is an underlying cause of your venous ulcers (i.e. varicose veins). From that scan and the knowledge that your ulcer is venous, the best course of treatment is defined for your case, tailored specifically to your condition.
We suggest that treating varicose veins with EVLA will produce the best long-term results. Once the treatment is complete and the veins have closed, the leg ulcer will heal relatively quickly as the underlying cause that led to the ulcer has been fixed. The wound will close up, the redness will fade, and any eczema will begin to clear up.
